You are using an out of date browser. It may not display this or other websites correctly.
You should upgrade or use an alternative browser.
You should upgrade or use an alternative browser.
America Shutdown Implemented To Ensure Our Healthcare Capacity Is Not Exceeded
- Thread starter Old Man Jingles
- Start date
Benben
Working on a new degree, Masters in BS Detecting!
Flattening the curve isn’t good enough
Pretty much sums it up unless you buy into the conspiracy theory that all hospitals are empty and all medical personnel are laid off!!!
Pretty much sums it up unless you buy into the conspiracy theory that all hospitals are empty and all medical personnel are laid off!!!
Poop Head
Judge me.
What if we flattened the curve so much, that it became like a bowl shape? What are the implications?Flattening the curve isn’t good enough
Pretty much sums it up unless you buy into the conspiracy theory that all hospitals are empty and all medical personnel are laid off!!!
Benben
Working on a new degree, Masters in BS Detecting!
What if we flattened the curve so much, that it became like a bowl shape? What are the implications?
More soup for U?
DriveInDriѵeOut
Inordinately Right
Great example of the shifting narrative of the extreme leftists. Nothing is good enough, orange man bad.Flattening the curve isn’t good enough
Pretty much sums it up unless you buy into the conspiracy theory that all hospitals are empty and all medical personnel are laid off!!!
Old Man Jingles
Rat out of a cage
That doesn't hold water!What if we flattened the curve so much, that it became like a bowl shape? What are the implications?
oldngray
nowhere special
That doesn't hold water!
Sportello
Well-Known Member
Once again, we have a winner!
Old Man Jingles
Rat out of a cage
What if, in theory, the curve doesn't come down, we plateau for months? How does that work out?
That's why I have been saying, regardless what politicians decide, I'm hibernating in my basement until a vaccine and/or therapeutic are developed.Once again, we have a winner!
Sportello
Well-Known Member
I haven't been anywhere there are people outside of my immediate household in two months. I'm not so sure there will be a vaccine or therapeutic this year. Possibly yes, probably no. The best minds in the world are working non-stop, so we will see.That's why I have been saying, regardless what politicians decide, I'm hibernating in my basement until a vaccine and/or therapeutic are developed.
Babagounj
Strength through joy
What are you going to do if a cure is never found ?I haven't been anywhere there are people outside of my immediate household in two months. I'm not so sure there will be a vaccine or therapeutic this year. Possibly yes, probably no. The best minds in the world are working non-stop, so we will see.
oldngray
nowhere special
What are you going to do if a cure is never found ?
Babagounj
Strength through joy
Massachusetts has opened up the Golf Courses with many restrictions. Club house are closed, along with rest rooms. No golf carts are allowed, only a hand cart that you bring with you can be used. Must reserve tee times by phone or online , payment is due when booking. Must wait in your vehicle until golf course notifies you. And when finished you have 15 mins to leave the area.
City of Lynn just had an accident , golfer broke a bone. Since no golf carts can be used there was a delay getting the victim off the course. Management had run back to the shop and get one.
City of Lynn just had an accident , golfer broke a bone. Since no golf carts can be used there was a delay getting the victim off the course. Management had run back to the shop and get one.
Babagounj
Strength through joy
I know the cure is four more years, followed by eight years with Pence as POTUS.
Sportello
Well-Known Member
Give you a big hug and a kiss!What are you going to do if a cure is never found ?
floridays
Well-Known Member
How about me darlin?Give you a big hug and a kiss!
Have you finished grading my paper yet?
Old Man Jingles
Rat out of a cage
Have we flattened the curve?
It’s too soon to declare victory, but it’s looking that way, says Dr. Stephen Hawes, professor of epidemiology at the University of Washington School of Medicine.
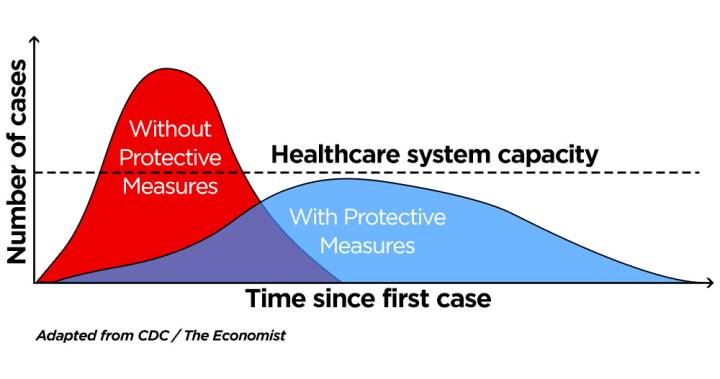
Even if the curve was flattened, it doesn’t mean the pandemic is over. Nationwide restrictions weren’t meant to reduce the number of cases of COVID-19. It was just to delay and spread them out over time. Rather than a steep peak of cases, a gentle, or flattened hill was the goal.
“It allows health departments and hospitals to be ready and not be overwhelmed with patients with COVID,” Hawes said. “The real worry early in the epidemic was how quickly this would ramp up and overwhelm the hospital staff and resources and ICUs.”
While the medical system has been able to take advantage of the slowdown in infections, so have other segments of society.
Businesses from restaurants to meat-packing plants are devising and implementing protocols designed to reduce infections between employees and the public.
“Flattening the curve also allows both medical professionals and businesses to learn what’s happening in other places and prepare for the best approach,” Hawes said. But the cost to businesses and workers has been enormous. Unemployment is the highest its been since the Great Depression. Even the medical industry has laid off and furloughed employees.
Testing is crucial in determining how widespread the pandemic has become, Hawes said. It’s the third type of test, serological, that most interests Hawes.
“It’ll be more about antibody testing to see who in the past has been infected, who might be immune,” Hawes said. “It’ll really inform what happened over the past two months in terms of transmission. What proportion of people were infected but didn’t have symptoms.”
For instance, testing could show how many young people were infected but were asymptomatic. Different policies could be developed for different demographics beyond the current ones that urge vulnerable groups to be more cautious.
Hawes understands that the public wants answers now. Widespread antibody testing will help, he said. “It’s frustrating, but we’re bound to learn more,” he said.
Social distancing is not only the most visible weapon in the fight against SARS-CoV-2, Hawes thinks it’s also the most effective.
“The fewer people that are infected who come into contact with uninfected people, the less likely we are to transmit it,” he said.
Masks are the proverbial two-way street. They can help prevent an infected person from spreading the disease, and they can help prevent an uninfected person from getting it. If you go out in public, it doesn’t matter which group you fall into.
“It doesn’t take much to wear a mask,” Hawes said. “It doesn’t take much to social distance.”

It’s too soon to declare victory, but it’s looking that way, says Dr. Stephen Hawes, professor of epidemiology at the University of Washington School of Medicine.
Even if the curve was flattened, it doesn’t mean the pandemic is over. Nationwide restrictions weren’t meant to reduce the number of cases of COVID-19. It was just to delay and spread them out over time. Rather than a steep peak of cases, a gentle, or flattened hill was the goal.
“It allows health departments and hospitals to be ready and not be overwhelmed with patients with COVID,” Hawes said. “The real worry early in the epidemic was how quickly this would ramp up and overwhelm the hospital staff and resources and ICUs.”
While the medical system has been able to take advantage of the slowdown in infections, so have other segments of society.
Businesses from restaurants to meat-packing plants are devising and implementing protocols designed to reduce infections between employees and the public.
“Flattening the curve also allows both medical professionals and businesses to learn what’s happening in other places and prepare for the best approach,” Hawes said. But the cost to businesses and workers has been enormous. Unemployment is the highest its been since the Great Depression. Even the medical industry has laid off and furloughed employees.
Testing is crucial in determining how widespread the pandemic has become, Hawes said. It’s the third type of test, serological, that most interests Hawes.
“It’ll be more about antibody testing to see who in the past has been infected, who might be immune,” Hawes said. “It’ll really inform what happened over the past two months in terms of transmission. What proportion of people were infected but didn’t have symptoms.”
For instance, testing could show how many young people were infected but were asymptomatic. Different policies could be developed for different demographics beyond the current ones that urge vulnerable groups to be more cautious.
Hawes understands that the public wants answers now. Widespread antibody testing will help, he said. “It’s frustrating, but we’re bound to learn more,” he said.
Social distancing is not only the most visible weapon in the fight against SARS-CoV-2, Hawes thinks it’s also the most effective.
“The fewer people that are infected who come into contact with uninfected people, the less likely we are to transmit it,” he said.
Masks are the proverbial two-way street. They can help prevent an infected person from spreading the disease, and they can help prevent an uninfected person from getting it. If you go out in public, it doesn’t matter which group you fall into.
“It doesn’t take much to wear a mask,” Hawes said. “It doesn’t take much to social distance.”
Similar threads
- Replies
- 94
- Views
- 16K
- Replies
- 2
- Views
- 2K
- Replies
- 178
- Views
- 28K

